Projects-publications

4C // COIMBRA COORDINATING CENTRE FOR CLINICAL RESEARCH

CEC // Clinical Trials Centre
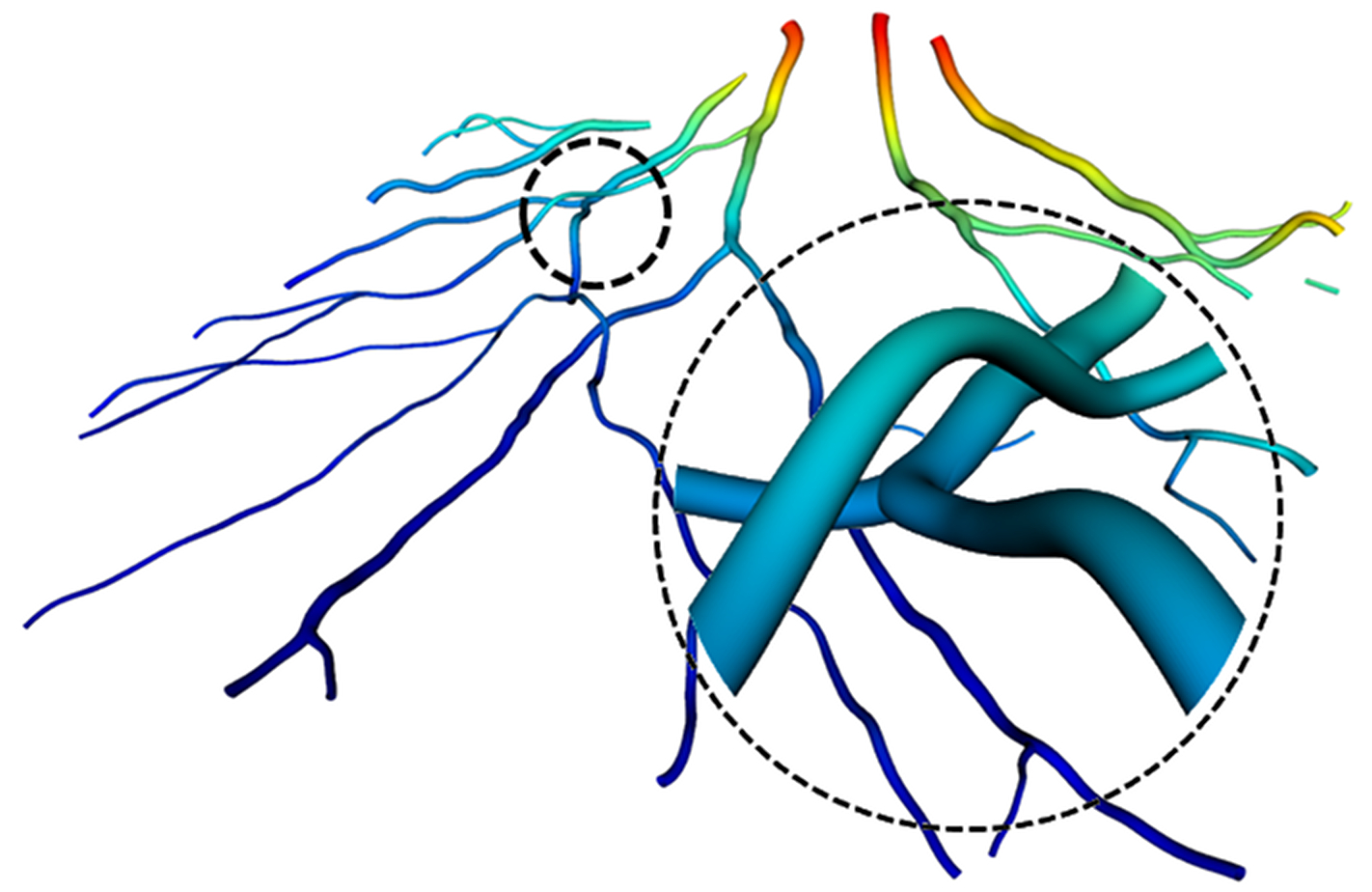
CNTM // Centre of New Technologies for Medicine
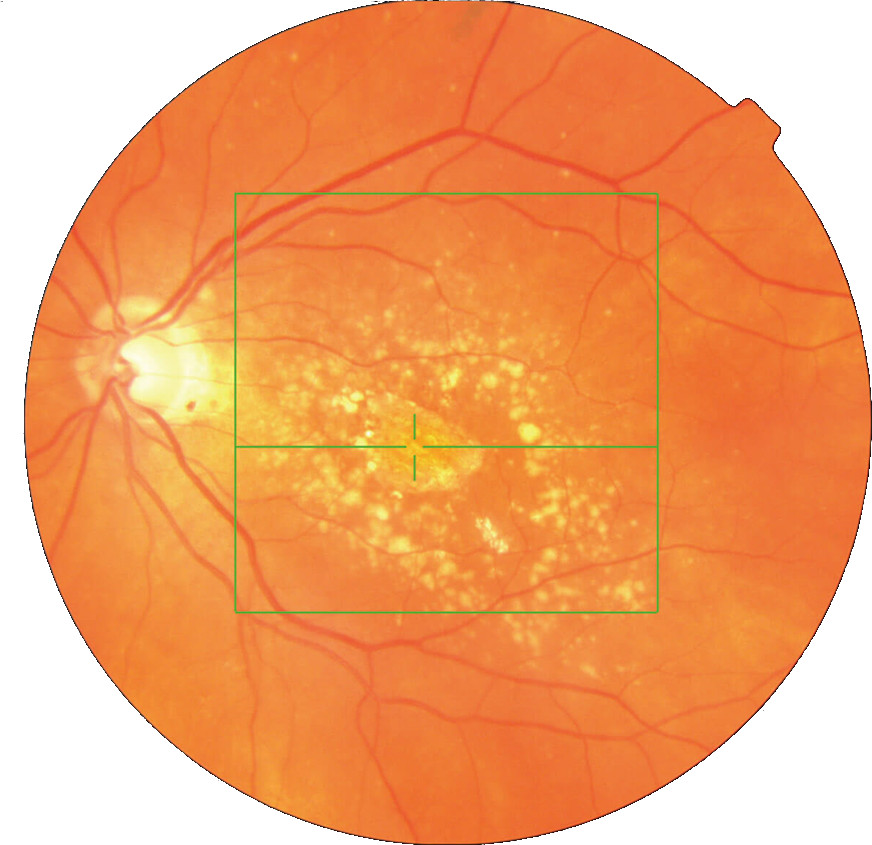
CORC // Coimbra Ophthalmology Reading Centre

DC // Datacentre

FUNDED PROJECTS

UFC // Pharmacovigilance Unit of Coimbra

usgi // Integrated Management System Unit